All 50 states required to audit 'high risk' Medicaid providers
Organizations that can demonstrate a rigorous, ongoing internal audit process are better positioned ...
OIG has audited Medicaid ABA payments in Indiana, Wisconsin, Maine and Colorado — and found improper payments in every one. The root cause was documentation. Here's what the findings show, and what ABA practices need to do now.
The federal government just released its fourth audit of Medicaid ABA payments since 2024 — and it’s the most consequential yet. Colorado’s audit found $285.2 million in confirmed and potentially improper payments, the highest total in the series so far. It’s a number that should catch the attention of every ABA provider billing Medicaid, regardless of what state they practice in.
ABA practices should also take note of the factors contributing to improper payment tallies. Across all four states, federal auditors aren’t finding evidence of widespread fraud. They’re finding documentation errors — the kind that are fixable, but only if providers catch them before OIG does.
Medicaid spending on ABA therapy has grown significantly over the past decade, driven by rising ASD diagnoses and expanded coverage mandates. Federal scrutiny has grown alongside, as the government has sought to vet new providers and get better visibility into care practices. In 2022, OIG announced it would audit ABA Medicaid payments across seven states, citing rapid spending increases and the potential for improper payments as the rationale.
Four of those seven audits are now complete. The findings have been remarkably consistent: in Indiana, Wisconsin, Maine and Colorado, 100% of sampled enrollee-months contained at least one improper or potentially improper claim line. Three more audits are still to come.
The four audits found hundreds of millions of dollars worth of improper or potentially improper payments.
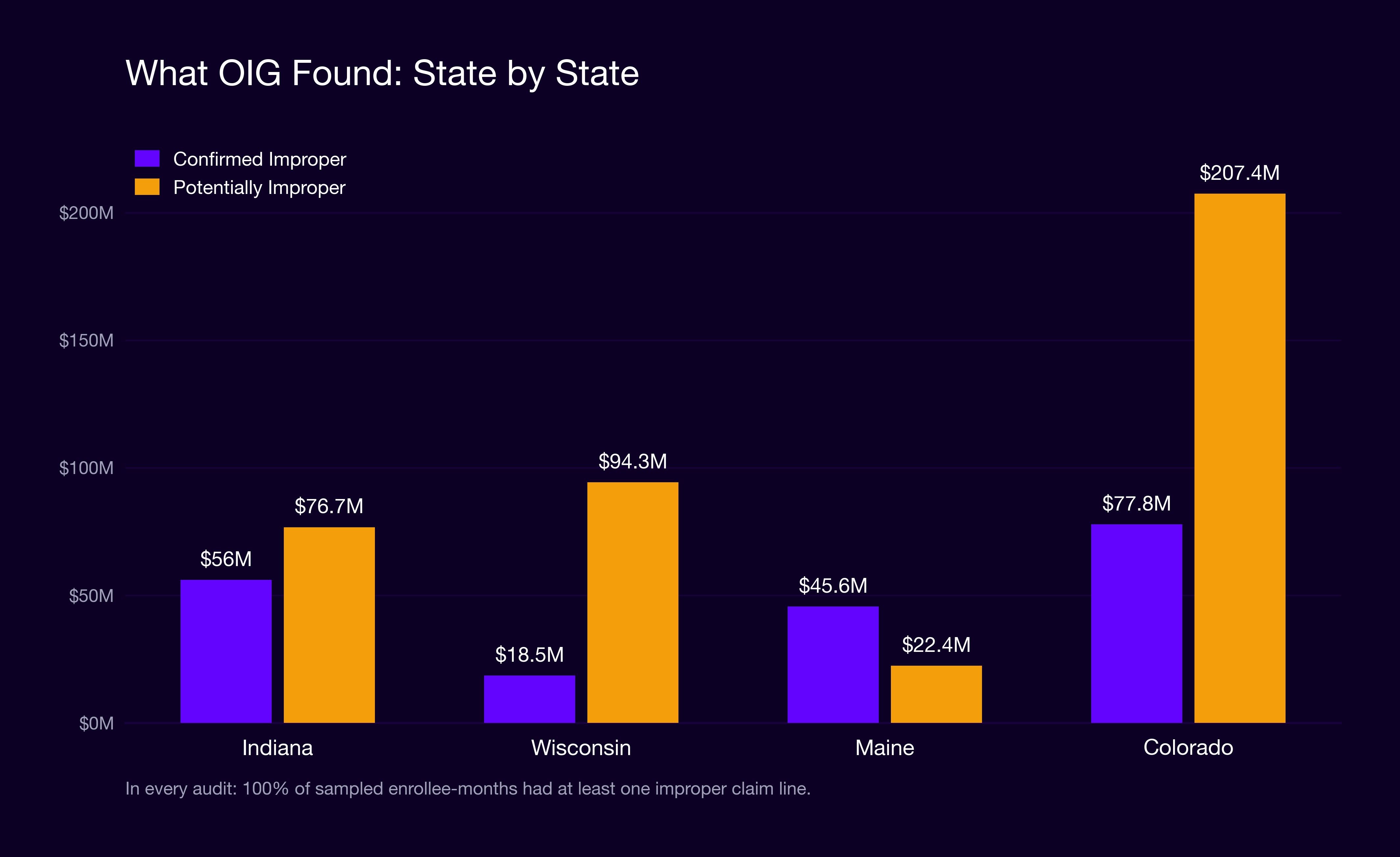
The root cause was the same across every state: documentation. OIG identified the following deficiency types consistently:
OIG’s recommendations were consistent as well: repay overpayments to the federal government, provide clearer guidance to ABA facilities on documentation requirements, implement statewide post-payment review processes, and ensure that claims reflect the credentials of the provider who actually delivered the service.
OIG committed to auditing seven states in 2022. With four complete and three pending, the series is only halfway through. ABA providers in any Medicaid-participating state should treat this as a live compliance risk, not a distant one. The documentation failures OIG is finding in Indiana, Wisconsin, Maine, and Colorado are not unique to those states.
These are fixable problems — but only if you invest in documentation quality and compliance. The providers most at risk aren’t necessarily doing anything wrong, but they don’t have a systematic process in place to make sure the care delivered matches what’s documented.
Brellium reviews every session note and treatment plan against your strictest funder’s latest requirements — before it becomes a denial. When something doesn’t hold up, we flag it early: so you can fix it upstream, before an audit letter arrives, and before a clawback.
That means checking for the exact issues OIG has flagged: CPT code support, unit documentation, provider signatures, non-therapy time, credential alignment. Not spot checks. Every note, every session.
Manual review doesn’t scale. One ABA provider group using Brellium reduced their auditing time by over 70% and eliminated the documentation errors that had been creating compliance exposure. Their clinical supervisors got back to doing what they trained to do.
We’ve worked with 170+ organizations. We know what funders look for. We know what holds up in audits. If you’re not confident your documentation does, that’s worth finding out now — before OIG does it for you.

Susanna currently works as Brellium's Content Marketing Director. She has previously held roles across healthcare, including as a journalist at Healthcare Dive, where she covered provider finances, care quality initiatives, and technological advancements. She also worked as a public policy researcher at Mathematica, conducting surveys for the DHA and SSA on Tricare and SSDI utilization and aiding the CMS in updating and maintaining Electronic Clinical Quality Measures.
AI-powered clinical compliance for every chart, every provider, every time.
Get a Demo